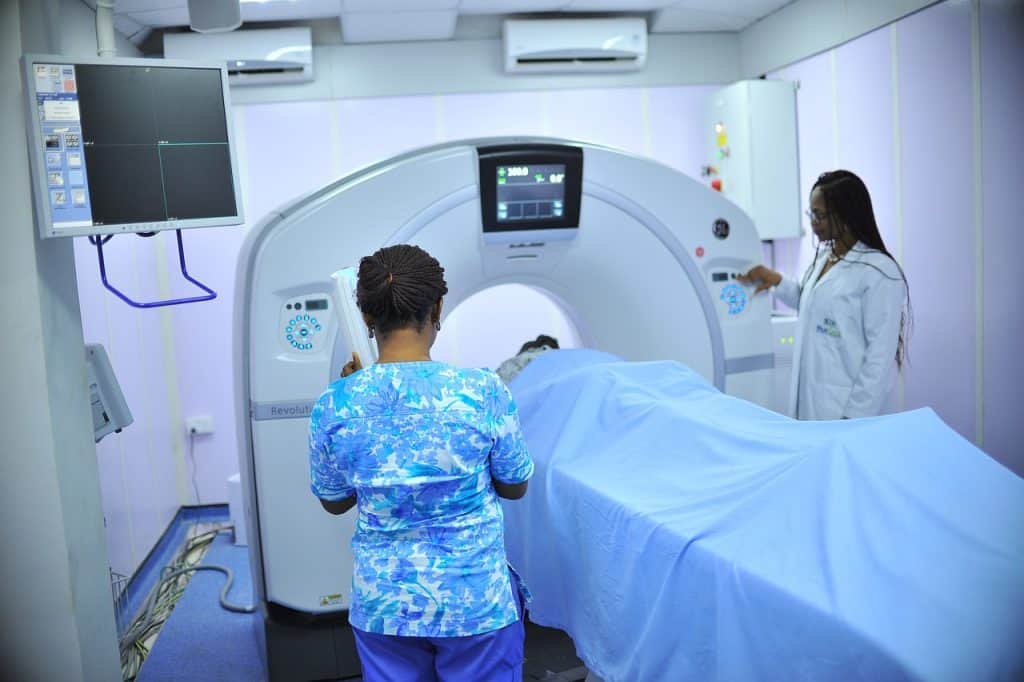
Imaging centers frequently wrestle with scheduling that feels like an uphill battle for both staff and patients. Limited scanner hours, high patient demand, and frequent changes to clinical priorities create a cascade of daily disruptions.
Staff at the front desk and in scheduling teams must balance clinical urgency, patient needs, and administrative checks while moving appointments around. Those tensions often lead to longer waits, missed revenue, and stressed teams.
High Demand And Limited Equipment Availability
Many centers run more patient requests than machine hours can comfortably absorb, creating a backlog that is hard to clear. A single MRI or CT scanner may serve multiple specialties and urgent inpatient needs, leading to tight windows for routine appointments.
When equipment is booked tightly any small delay ripples through the day and forces staff into reactive rearrangement. Supply of machine time rarely matches the steady stream of orders that land in scheduling queues.
Variability In Exam Duration And Complexity
Not every scan fits the same time slot and some studies expand beyond initial estimates on the fly. Exams may require contrast injection, additional sequences, or longer image acquisition when unexpected findings appear.
Booking a fixed block for a variable task creates idle time in some cases and overrun in others, which complicates batching and flow. Many imaging departments therefore rely on scheduling platforms built for high-volume exam scheduling to better account for these differences and keep the calendar balanced.
Prep Requirements And Patient Readiness
Certain procedures require fasting, medication changes, or arrival at a precise window to be valid and safe for imaging. When preparation instructions are missed or misunderstood patients arrive late or unprepared and an open slot evaporates.
Rescheduling for correct prep involves juggling clinical priority and patient convenience while trying to keep scanners productive. Clear directions help, yet human error in remembering steps keeps no shows and delays on the schedule.
Fragmented Referral And Scheduling Workflows
Referrals often come through multiple channels that do not talk to one another, such as faxed orders, portal submissions, or phone calls. That fragmentation forces schedulers to verify clinical indications, confirm availability, and map imaging needs to the right protocol before an appointment is placed.
Time spent on manual checks and clarifying orders reduces capacity for proactive scheduling and creates bottlenecks. The result is slower turnaround from order to appointment and more room for error.
Staffing Shortages And Turnover
Scheduling requires experienced staff who can triage requests, match protocols, and manage patient expectations with care. High turnover and vacancies leave fewer hands doing more work which amplifies mistakes and slows response time.
Training new team members on nuanced protocols and insurance needs takes time that already stretched teams do not have. When human resources are thin the calendar becomes a fragile thing that bends at the first gust.
Insurance Prior Authorization And Billing Delays
Many scans require preauthorization or verification that benefits cover the indicated study, which can take hours or days to process. While a patient waits for clearance the appointment cannot be reliably confirmed and open blocks sit unused or get filled last minute.
Billing denials returned after the fact force rework and rescheduling that eats administrative time. Authorization work pulls schedulers away from proactive outreach and slot optimization.
Patient No Shows And Late Arrivals

Patients sometimes miss appointments due to transport, work conflicts, or simple forgetfulness and that empty chair costs the center real revenue. When a patient arrives late the technologist may only be able to do part of the exam or have to shift the next slot around, creating a chain reaction.
Many centers try reminder calls and texts yet a single failure can throw a roster into disarray. The uncertainty of whether a patient will show up makes planning feel like guesswork.
Communication Gaps Between Teams
Radiology technologists, schedulers, front office staff, and referring clinicians all need to share accurate and timely information to keep a day on track. Miscommunication about prep, urgency, or protocol requirements forces last minute changes that ripple through the schedule.
When messages are buried in emails or spread across multiple platforms valuable context gets lost between handoffs. A missed note can lead to wasted scanner time and frustrated patients.
Outdated Or Inflexible Scheduling Software
Many centers still rely on legacy systems that are hard to modify for new protocols or specialty needs and that do not reflect real world constraints. Rigid calendars that lack smart buffering or adaptive slotting force staff to do manual juggling that increases cognitive load.
Software that fails to reflect actual exam lengths or that cannot flag prep requirements contributes to misbookings. The tech ought to be a partner in smoothing flow yet often becomes a source of friction.
Emergency And Urgent Case Interruptions
Hospitals and some outpatient centers must accommodate urgent inpatient studies and post procedure scans that jump the queue and take precedence. When emergencies appear the elective schedule gets carved up and routine patients are moved, a process that is never popular.
Triage of who gets bumped requires clinical judgment and coordination that costs time and emotional labor. The unpredictability of urgent work keeps the calendar in a near constant state of flux.
Financial Pressures And Productivity Targets
Centers carry pressure to hit utilization numbers and revenue targets that push staff to double book or squeeze extra appointments into thin windows. That tactic can raise short term yield yet it erodes trust when patients experience delays or shortened encounters.
Management expectations for throughput without matching resources create tension that shows up in scheduling choices. When financial metrics dominate the agenda scheduling becomes an arithmetic exercise rather than a patient centered plan.